Gastric band complications are common and can necessitate revision or conversion surgery, sometimes several years after the initial procedure.
Although adjustable gastric bands were once a popular weight loss option, they can cause issues such as slippage, erosion, significant reflux with persistent vomiting or inadequate weight loss over time.
In many cases, this requires medical attention and, in most instances, surgical removal of the band.
Gastric Band Problems
Common Gastric Band Problems
Gastric bands are associated with a range of mechanical and functional issues, including:
- Band slippage
- Band erosion into the stomach
- Food intolerance or persistent vomiting
- Acid reflux or heartburn
- Difficulty swallowing (dysphagia)
- Port or tubing malfunction
- Inadequate or failed weight loss
These problems often worsen over time rather than resolve spontaneously.
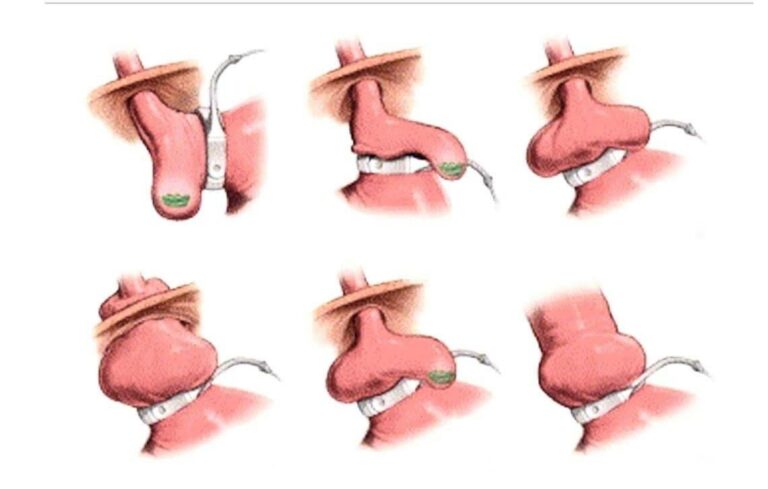
Gastric Band Slippage
Band slippage occurs when part of the stomach moves above or below the band, altering its position. This can lead to obstruction and significant symptoms.
Common signs of band slippage include:
- Sudden onset of vomiting
- Inability to tolerate solid or liquid food
- Chest or upper abdominal pain
- Reflux or regurgitation
Band slippage is not usually correctable with simple band adjustment and often requires surgical intervention.
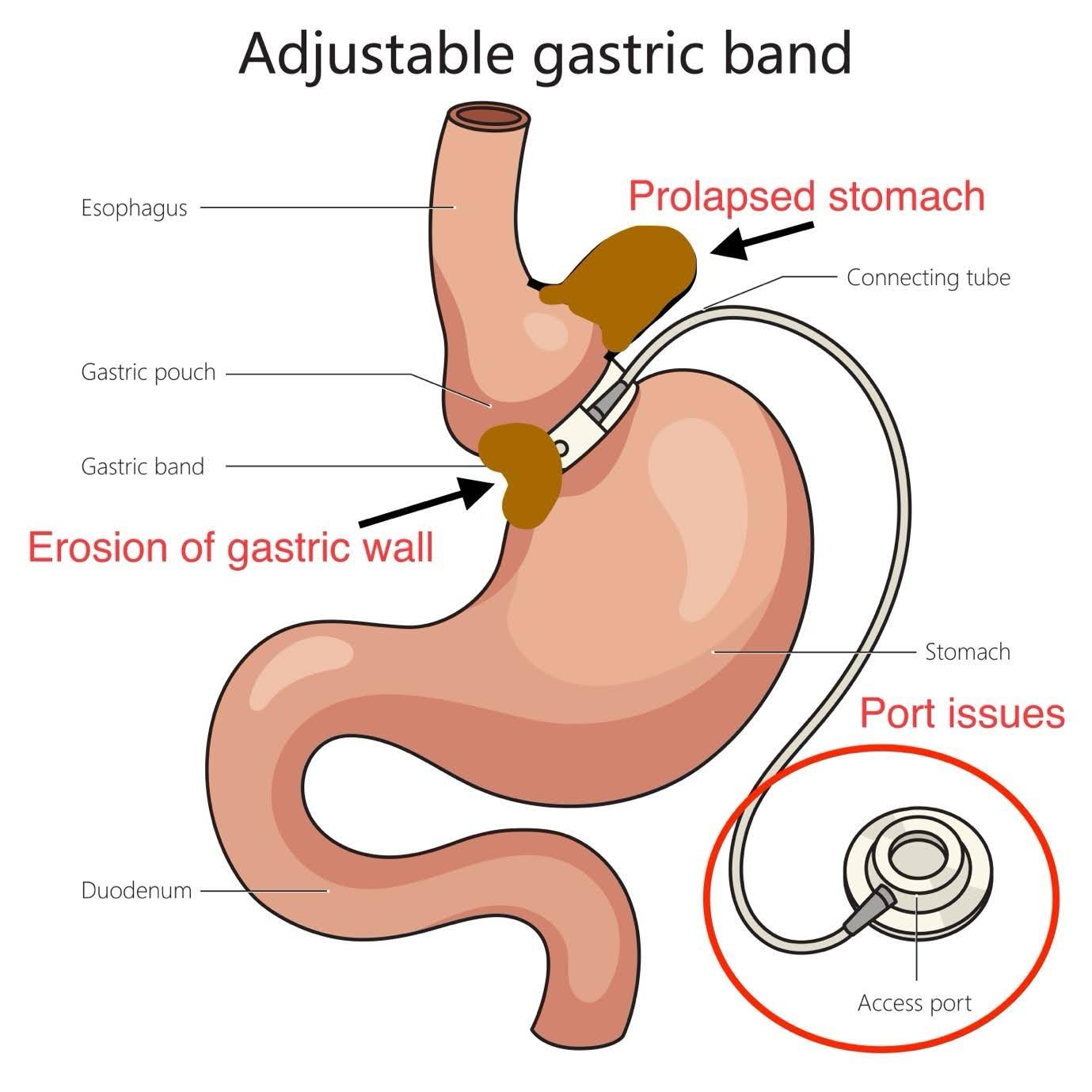
Band Erosion
Band erosion is when the gastric band slowly wears down the stomach wall, sometimes embedding itself partially inside. It is not very common, but spotting it early is super important.
Possible causes:
- Intraoperative Trauma: Small, unrecognised injuries to the stomach wall during placement can weaken tissue, while excessive dissection around the stomach can compromise blood supply, increasing the risk of erosion.
- Chronic Pressure from an Overtightened Band: Constant high pressure on the stomach wall can impair blood flow, and over-restriction or repeated aggressive tightening increases the risk.
- Infection Around the Band or Port: Chronic low-grade infections can track along the tubing and weaken the gastric wall, and recurrent port-site infections are sometimes associated with erosion.
- Use of NSAIDs: Drugs like ibuprofen, naproxen, and diclofenac can cause gastric irritation and ulceration, which can lead to erosion through the stomach wall.
- Repeated Vomiting or Dysphagia: Persistent vomiting can cause microtrauma and pressure changes, while chronic inflammation can weaken the tissue around the band.
- Foreign Body Reaction: Some patients develop a chronic inflammatory response to the silicone band, which can thin or damage the stomach wall.
- Ischaemia (Reduced Blood Supply): If the band compresses small blood vessels supplying the stomach, tissue integrity declines, and scar tissue formation may worsen over time.
- Improper Band Position or Migration: A band placed too tightly or too close to the gastro oesophageal junction may stress tissues unevenly, allowing the band to dig into the stomach wall.
- Long Duration in Situ: Erosion risk increases the longer the band remains in place, and many erosions occur years after insertion as the stomach slowly adapts and thins around the device.
Possible Symptoms
-
- Loss of restriction, allowing larger quantities of food to be eaten without feeling full
- Frequent infections around the port site
- Chronic abdominal discomfort
- Bleeding, which may be observed as dark or tarry stools
- Unexplained weight regain
- Nausea or vomiting
- Loss of fluid from band system
- Asymptomatic (incidental finding during endoscopy for another reason)
Diagnosis
Diagnosis is usually confirmed by endoscopy, which enables direct visualisation of the inside of the stomach.
Treatment
- Surgical (or endoscopic- if feasible) removal of the band is required
- Additional repair surgery may be needed depending on the extent of tissue damage
When Gastric Band Removal Is Recommended
Gastric band removal is advised when complications persist or when the band no longer provides benefit. Indications for removal include:
- Recurrent or severe vomiting
- Band slippage or erosion
- Chronic reflux or esophagitis
- Mechanical failure of the band system
- Poor weight loss or weight regain
- Patient intolerance or reduced quality of life
Removal prevents further damage to the stomach and esophagus.
Gastric Band Removal Surgery
Gastric band removal is typically performed laparoscopically under general anaesthesia. The procedure involves removing the band, port, and tubing, and carefully restoring normal stomach anatomy.
In some cases, band removal may be:
- Standalone surgery, with no immediate replacement
- Combined with delayed conversion surgery, such as gastric sleeve or gastric bypass, depending on patient suitability
The surgical approach is individualized based on symptoms, anatomy, and prior complications.
Recovery After Band Removal
Recovery after gastric band removal is usually quicker than the original bariatric procedure:
- Most patients go home the same day or after one night
- Gradual return to normal diet as advised
- Temporary bloating or discomfort may occur
- Return to daily activities within 1–2 weeks
If a conversion procedure is planned, recovery follows bariatric surgery protocols.
Risks and Considerations
Gastric band removal is generally safe, but potential risks include:
- Bleeding or infection
- Stomach or oesophageal injury (rare)
- Scar tissue or adhesions
- Weight regain if no further bariatric strategy is planned
Careful surgical technique and appropriate follow-up reduce these risks.
When to Seek Medical Advice
Medical review is recommended if you experience:
- Persistent vomiting or reflux
- Difficulty swallowing
- Chest or upper abdominal pain
- Sudden inability to eat or drink
- Weight regain with band-related symptoms
Why Mr. Spyros Panagiotopoulos?
With years of experience in metabolic and bariatric surgery, as well as acute surgery, Mr Panagiotopoulos is well-equipped to offer the best solution for your needs. By collaborating closely with a team of experts, we will use treatments that are supported by research and provide strong follow-up to help you achieve your goals.

